The risks posed by asbestos have been well known for most of the 20th century. It is widely accepted that exposure to varying amount of asbestos can cause mesothelioma and lung cancer.
Insurers and actuaries have long debated whether we are over the peak of asbestos-related mesothelioma claims, but based on the Work and Pension Select Committee’s recommendation to remove asbestos from all buildings by 2062, the potential for exposure remains for the foreseeable future. What’s more, given the latency period between exposure and manifestation of 20 to 30 years, this suggests that asbestos-related mesotheliomas remains a possibility until 2092.
The current data on mesothelioma deaths
However, the numbers of mesothelioma have long been monitored by actuaries as the best way to predict future claims numbers. The Faculty of Actuaries has published the following scenario:
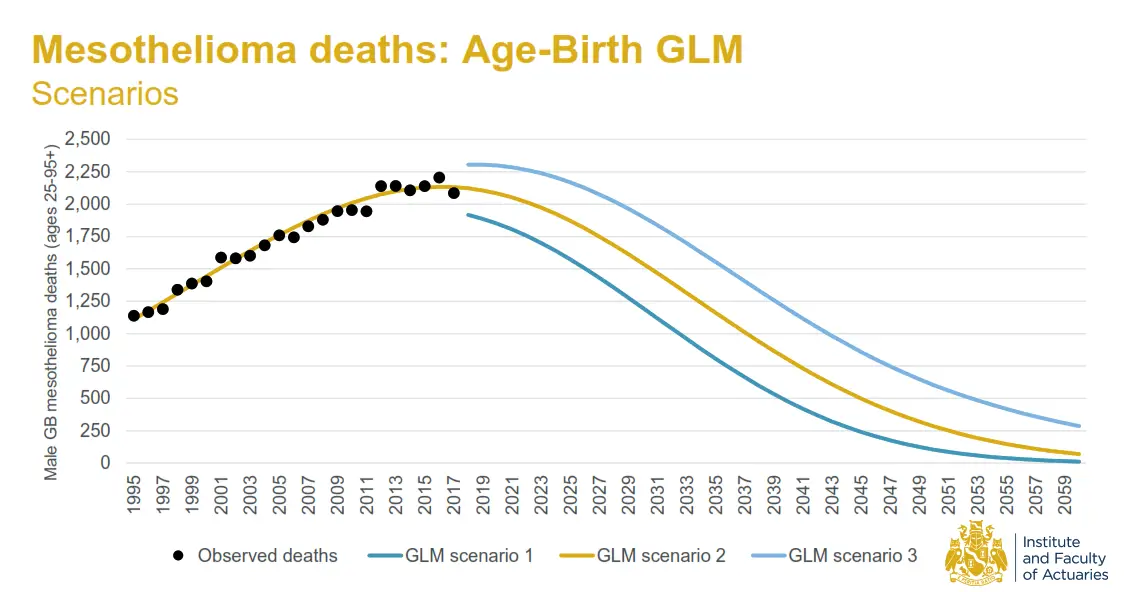
Source: Institute and Faculty of Actuaries, UK Asbestos Working Party update, September 2019
Based on the best data available for mesothelioma it is reasonable to say that claims numbers, from their 2019 peak, are due to half by around 2039 and largely disappear by 2059. Whether this comes to pass is a point of debate.
The Department of Work and Pensions in 2014 found the average legal costs paid for a mesothelioma claim to be in the region of £30,000, giving an annual cost to insurers of approximately £72 million. Given the sums relating to costs recovered by bringing these claims, this market has consolidated into an efficient space with four large firms acting for a majority of asbestos victims and national coverage by various asbestos victims charities.
However, in the coming 20 years these firms face declining claims numbers and revenues as we travel further down the mesothelioma tail. The challenge for insurers will be to identify where new challenges present themselves to stop expansions of future liabilities not supported by medical evidence.
In this article, we look at two recent developments in this area; carcinoid tumours and head and neck cancers.
Carcinoid tumours
Carcinoid tumours are made up of neuroendocrine cells found throughout the body which develop from uncontrolled growth of neuroendocrine. They can usually be treated with surgery and chemotherapy and often the prognosis is more positive than other types of lung cancer.
Recently small numbers of claims have been brought trying to implicate asbestos as a cause of carcinoid tumours by relying on a 2012 French study ‘Pulmonary Carcinoid Tumours and Asbestos Exposure’. The study noted that in 28 carcinoid tumour patients, 25% (seven patients) had a history of exposure against a control group of 14%. On this small cohort, the paper concluded that there is a relationship between asbestos and carcinoid tumours. However, the paper did not consider:
- A number of other papers involving larger groups suggesting that asbestos exposure does not increase the risk of developing a carcinoid tumour.
- The limitations of the small study group, the problems of accurately recording exposure and lack of a proper control group.
- Even if there was an association the lack of evidence to show a dose response relationship, at what point of exposure there is a doubling of the risk (the necessary threshold to satisfy legal causation).
Given the issues above, in our view there is presently an unsound basis to support these legal claims and as such, they should be rejected.
Head and neck cancers
In March 2022, a large-scale study called ‘Head and Neck Cancer and Asbestos’ was published. The study concluded that there is a relationship between a number of head and neck cancers (beyond laryngeal cancers) and prior asbestos exposure. According to the authors, the study “could lead to new recommendations for occupational medical surveillance of workers previously occupationally exposed to asbestos, and to new modalities concerning the potential medico-legal compensation for associated cases of head and neck cancers, other than laryngeal cancers”.
Unlike the evidence for carcinoid tumours, this was a large-scale longitudinal study involving over 13,000 individuals monitored over 10 years. It found that a “dose-response relationship” existed with or without the presence of pleural plaques. This latter finding is particularly concerning because the dose-response relationship was established without the presence of pleural plaques, which suggests very low levels of exposure could be implicated. However, further research is recommended before changes are made to the medico-legal landscape.
With the NHS making 12,500 head and neck cancer diagnoses each year, this is a worrying development given the large pool of potential claimants. Of course, this pool will be vastly reduced by the diminishing potential for exposure to asbestos but a sizable number could remain if the levels needed to double the risk are low. Any follow up studies in this area that explore this relationship will require careful consideration.
Comment
It is thought by many that the long legacy of asbestos is beginning to pass with insurers and reinsurers facing the downwind tail.
Today, in our view, the science is not sufficient to support some of the new claims being brought, as above, but it remains to be seen what tomorrow’s research will find.
 United Kingdom
United Kingdom